Diabetic Kidney Disease - Averting End Stage Renal Disease Through Early Detection
Diabetes can wreak havoc on the kidneys' filtering system, resulting in diabetic kidneydisease. The kidneys are unable to remove waste products effectively in this condition, and toxic levels of residue can accumulate in the body.
This can lead to serious health issues, such as kidney failure, and, if left untreated, could be life-threatening.
As a result of the worldwide diabetes epidemic, diabetic kidney diseasehas become more common. Diabetic kidney disease can lead to serious complications, including renal failure in various stages.
In the future, this could result in the emergence of cardiovascular diseases such as heart attack and stroke. It's crucial to evaluate the kidney's functional capacity and monitor the disease's progression in diabetic kidney disease.
The most difficult challenges are early detection and prevention of progression, which will help diabetic kidney disease patients live longer.
What Are The Symptoms Of Diabetic Kidney Disease?
There are typically no symptoms at all in the early stages of kidney disease. Urine and blood tests are typically the only ways to detect early kidney disease. Kidney disease usually does not manifest itself until kidney function is nearly gone.
Many symptoms are indistinct even when the kidneys are severely damaged. Regular blood sugar and urine protein tests, as well as lab tests to check for a buildup of waste products, are essential.
Diabetic nephropathy can cause the following symptoms in late stages:
- Loss of sleep
- Poor appetite
- Weight loss
- Nausea
- Weakness
- Trouble concentrating
- Dry, itchy skin
- Muscle cramps
- Increased urination
- Fluid accumulation (swelling in the ankles or feet or hands)
- Puffy eyes
Diabetic kidney disease
What Are The Causes Of Diabetic Kidney Disease?
When blood sugar levels remain high, as they do in poorly controlled diabetes, the kidneys filter an excessive amount of blood.The additional work puts a strain on the kidney's filtering system. The filters begin to leak over time, resulting in the loss of valuable protein (which is then excreted in the urine).
Microalbuminuria is a condition in which a small amount of protein is detected in the urine. Macroalbuminuria is a condition in which the urine contains a large amount of protein. Microalbuminuria is a treatable stage of kidney dysfunction, but macroalbuminuria is usually followed by end-stage kidney (renal) disease (ESRD). ESRD is a life-threatening condition that may necessitate dialysis or a kidney transplant.
Some Clinical Reports On Diabetic Kidney Disease
Diabetic kidney disease is a chronic condition that develops over time, according to previous research. On the other hand, certain diabetic patients' renal function rapidly deteriorates. If not caught and treated early enough, this can quickly develop into chronic kidney disease and, eventually, end-stage kidney failure. Renal failure prevention becomes more difficult as a result.
Over the last two decades, numerous pathways associated with the pathogenesis of diabetic kidney disease involving a multifactorial interaction have been extensively investigated; however, the precise mechanism underlying this interaction remains unknown. Interactions between metabolic and hemodynamic pathways, which frequently include glomerular hyperfiltration, progressive albuminuria, and declining glomerular filtration rate, have been reported to play a role in the pathogenesis and progression of diabetic kidney disease.
Hyperglycemia and hyperaminoacidemia, both of which promote glomerular hyperfiltration and hyperperfusion, cause changes in renal hemodynamics and promote inflammation and fibrosis in early diabetes, are metabolic changes that cause a change in renal hemodynamics. The symptoms of these metabolic changes include glomerular hypertrophy, glomerulosclerosis, tubulointerstitial inflammation, and fibrosis. Additionally, due to increased production of reactive oxygen species, oxidative stress is thought to play a role in the progression of diabetic kidney disease.
According to studies, the severity of microvascular diabetic complications is strongly linked to urinary oxidative DNA damage biomarkers. The basement membrane of the glomerulus thickens, endothelial fenestrations disappear, the mesangial matrix expands, and podocytes disappear.
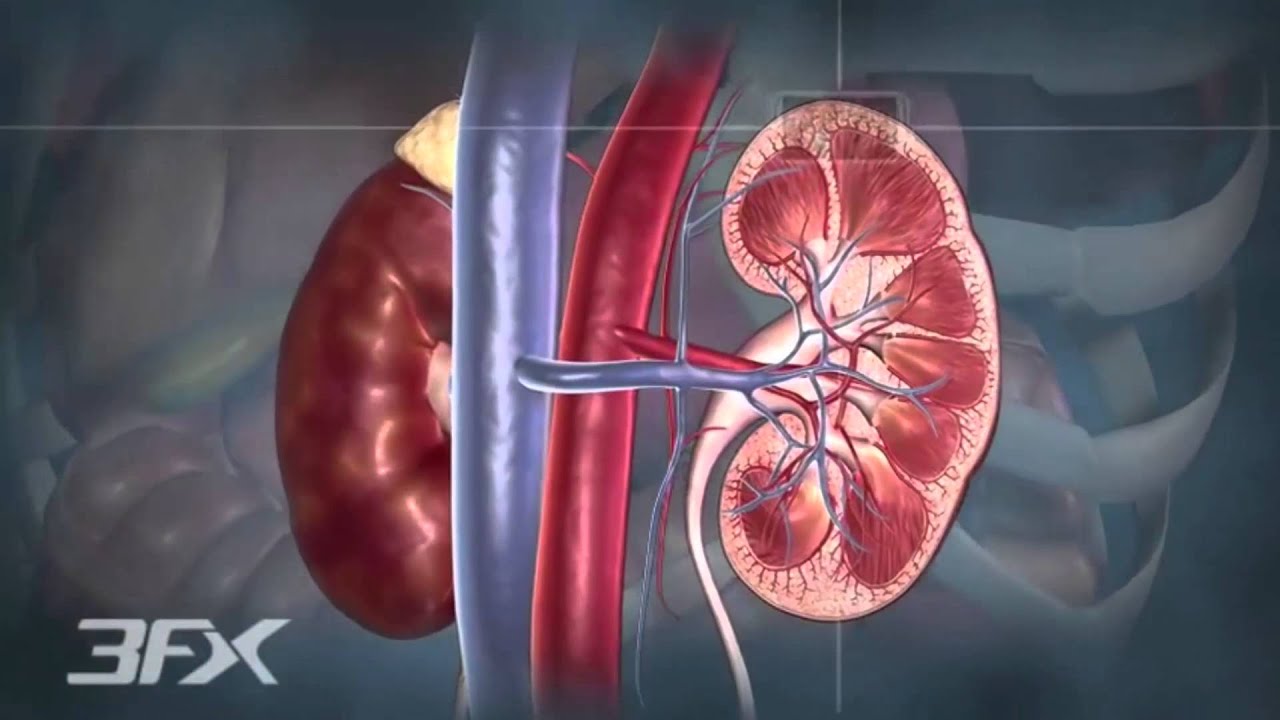
How can Diabetes affect your Kidneys?
Modern Diagnostic Tools Used To Detect Diabetic Kidney Disease
Among the most advanced diagnostic tools available today are novel biomarkers for detecting diabetic kidney disease progression and early therapeutic intervention to prevent kidney damage before a decrease in glomerular filtration rate and albuminuria. Some of the possible biomarkers that have been reported in studies in the diagnosis of chronic kidney disease include glomerular and tubular injury biomarkers, inflammation biomarkers, and oxidative biomarkers that precede albuminuria in some patients and may thus be useful for the early detection of diabetic kidney disease.
A number of urinary biomarkers have been proposed as more sensitive diagnostic tools for early detection of diabetic kidney disease and progression to end-stage kidney disease. Tubular dysfunction occurs before microalbuminuria and glomerular injury, so tubular biomarkers have been identified as primary predictors of diabetic kidney disease.
Urinary tubular biomarkers, urinary microRNAs that regulate gene expression, and urine proteomics are all elevated before microalbuminuria appears, implying that epigenetic factors may play a role in disease progression. The routine use of these biomarkers in future clinical trials would aid in the diagnosis of various stages of diabetic kidney disease and would result in a better diabetic kidney disease outcome with a more effective therapeutic approach. These biomarkers are still used in clinical trials, and their accuracy must be determined.
Researchers are focusing on new therapeutic interventions and techniques to prevent complications of diabetic kidney disease and progression to end-stage renal failure. Diabetic kidney disease is still one of the leading causes of end-stage renal failure, and it is estimated that 40% of diabetic patients will develop the disease, resulting in a significant population requiring renal replacement therapies for end-stage renal failure, which is a significant socioeconomic and public health issue.
How Can Diabetic Kidney Disease Be Prevented?
Prevention measures, such as a healthy lifestyle, are perhaps the most effective way to manage diabetic nephropathy. This allows the healthcare provider to detect kidney problems early on, when there are more treatment options.
According to research, maintaining strict blood sugar control has been shown to reduce the risk of microalbuminuria and the risk of microalbuminuria progressing to macroalbuminuria.
The following are some of the steps you can take to lower your risk of developing kidney disease:
- Smoking should be avoided at all costs. Cigarettes have been shown to harm the kidneys and to exacerbate any existing kidney damage. It's critical to take steps to quit smoking if you are a smoker. Consult your doctor about any medications that might help you quit smoking, and think about joining a support group or other types of groups, as well as individual or group therapy.
- Maintain a healthy weight by exercising regularly and eating nutritious foods. Maintain an active lifestyle by working out on a regular basis. Limit your intake of processed foods, sugar, saturated fats, and other unhealthy foods by eating a healthy diet. Consult your healthcare provider about weight loss options if you are overweight.
- Take medications with caution. Some medications, such as over-the-counter pain relievers like ibuprofen and others, can cause kidney damage if they are not taken as prescribed. Any medications, vitamins, or herbal supplements you are taking should be discussed with your healthcare provider.
- Keep your blood pressure under control. Diabetes and high blood pressure are the leading causes of kidney failure. Diabetic kidney disease is frequently accompanied by hypertension. The effects of hypertension on the kidneys can be amplified. Even a small increase in blood pressure can aggravate kidney disease.
- Maintain regular diabetes treatment.
People Also Ask
What Is The Most Important Symptom Of Early Kidney Disease From Diabetes?
Increased albumin excretion in the urine is the first sign of diabetes-related kidney disease.
Why Do Kidneys Fail In Diabetes?
The millions of tiny filtering units within each kidney are damaged over time by high levels of sugar in the blood. Kidney failure develops as a result of this. Diabetic nephropathy affects 20 to 30% of people with diabetes, but not everyone develops kidney failure.
What Happens To Kidneys With Diabetes?
Diabetes can harm your kidneys by causing damage to the following blood vessels: blood vessels within your kidneys. The kidney's filtering units are teeming with small blood vessels. High blood sugar levels can cause these vessels to become narrow and clogged over time.
What Occurs During The Early Stages Of Diabetic Kidney Disease?
A person with diabetic nephropathy may not experience any symptoms in the early stages. Changes in blood pressure and fluid balance in the body, on the other hand, could already be present. Waste products can accumulate in the blood over time, causing symptoms.
Conclusion
It's important to remember that once the kidneys fail due to diabetic kidney disease, dialysis or a kidney transplant are required. At this point, it's best to consult with a group of diabetes specialists as well as kidney specialists. A nephrologist is a doctor who specializes in treating kidney problems. A kidney transplant surgeon, a social worker, and a diabetic educator (such as a nurse who is specially trained in diabetic teaching) should all be on the team.
